Measles Is Back on the Faculty Meeting Agenda
How one of the most contagious viruses on Earth spreads through schools—and why we’re talking about it again.
We’re going to party like it’s 1959!
The faculty meeting the week before spring break had the usual vibe: it could’ve been an email. Announcements, schedule reminders, and the usual odds and ends. Then we got to the item that changed the mood of the room: measles. Not a hypothetical. Not a public-health bulletin somewhere else. Our district believes it’s coming here.
Our school nurse (technically not our nurse—she rotates among several schools, but that’s a conversation for another day) got up and delivered the presentation the district had prepared.
The short version:
Measles cases are rising in our part of the country, and as far as the district is concerned, arrival here isn’t an if but a when.
My school is reasonably well-protected, though we do have a few students who aren’t vaccinated. Thankfully, in North Carolina, we still require immunizations for students to attend public school.
Symptoms, transmission, and oh holy God does this thing spread.
Regular readers know I don’t often find myself nodding along with whatever floats down from the district office. But on this one, they were probably right. It’s coming.
Okay.
Look, I like our school nurse a lot. She’s competent, thoughtful, and trying to do an important job with very little support. So she did what she could. A few slides. A few reminders about symptoms. Some procedures if a suspected case appears.
But, as with most faculty meetings, the presentation answered some questions and raised a dozen more. You could feel it in the room. People were half-listening, half-checking email, half-trying to figure out whether this was something they actually needed to worry about. Questions ranged from the predictable—things already covered in the slides—to speculation better suited for a hyperbolic Facebook thread.
Then one detail landed: if a teacher is exposed to measles and can’t show documented immunity, the exclusion window is twenty-one days. And, depending on the situation, that time might not be paid leave.
A week later, the district followed up with an email that felt like HR and legal had written it while gently elbowing the employee health people out of the room.
To be fair, I’m not sure if we have employee health people.
The email was straightforward: measles is rising, and staff should locate their vaccination records. If we’re exposed and can’t show proof of immunity, we could be excluded from work for twenty-one days.
The instructions that followed had a distinctly archaeological feel.
Check with your doctor.
Ask your parents.
Look in your baby book.
Contact schools you attended decades ago.
Reach out to health departments in other states if you’ve lived elsewhere.
In other words: start digging. If records can’t be found, the district suggested the simpler solution—just get another dose of the vaccine. Pharmacies and health departments can administer the MMR (measles, mumps, rubella) vaccine quickly.
That was the option I had already taken during the meeting itself.
Look, we don’t tend to keep teachers around that long anymore (I wrote a whole article about it), so at fifty-six, I have no realistic hope of locating my childhood immunization paperwork. Somewhere, at some point in the early 1970s, a pediatrician almost certainly wrote something down on a card that has long since disappeared into the deep sedimentary layers of family paperwork.
So while the nurse was presenting slides about measles symptoms, I scheduled an MMR booster at Walgreens. It took about two minutes.
Got the shot the next day. Two doses of the MMR vaccine provide about 97% protection against measles, so a small leap of faith that I’ve already had one (I’m sure I did), but I’m good to go.
But being the science nerd (and teacher) I am, I went down the measles rabbit hole.
The Measles Science Stuff
Let’s start with the part the meeting didn’t really unpack very well: what measles actually is.
Measles is caused by a paramyxovirus—a nasty family of viruses that includes mumps and distemper in animals. It spreads through the air when an infected person coughs, breathes, or even just talks. The virus can linger in a room’s air for up to two hours after the infected person leaves.
In fact, about 90% of unvaccinated people exposed to measles will become infected.
Imagine a classroom with twenty-five students. If one student walks in contagious with measles and nobody is vaccinated or immune, twenty of them could end up infected. That’s not a dramatic exaggeration. That’s the math.
Epidemiologists measure contagiousness using the basic reproduction number, written as R₀. It represents the average number of people one infected person infects in a population with no immunity.
Seasonal flu usually has an R₀ around 1–2.
The original strain of COVID-19 was roughly 2–3 (though that later rose, with the Omicron variant topping out at near 10).
Measles lives in a completely different league.
Its R₀ is usually estimated at 12–18.
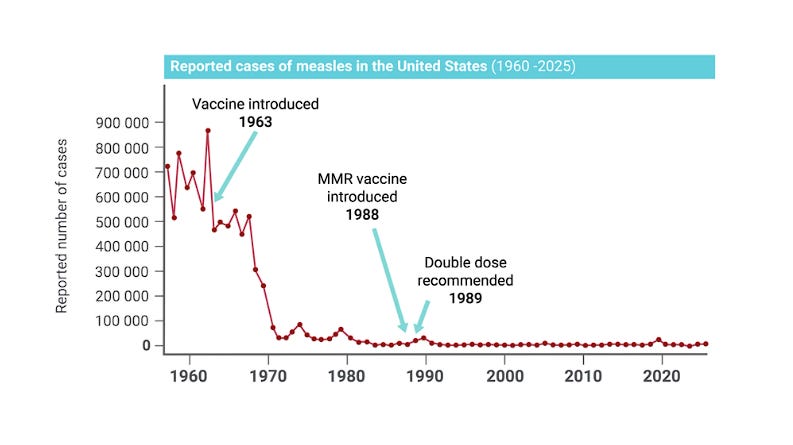
Before the vaccine was introduced in 1963, measles infected hundreds of thousands of Americans every year, hospitalizing about 48,000 and killing 400–500 children annually.
In epidemiology terms, measles is basically the Michael Jordan of contagious diseases.
Very few human diseases spread that efficiently.
That’s why measles was a routine childhood illness (albeit with occasional life-long complications and fatalities) before 1963, and why outbreaks still spread quickly when they find pockets of low vaccination coverage.
On the “plus” side, we know this virus well. Measles has been circulating in North America since the colonial era. Interesting fact — In 1988, Roald Dahl wrote a public letter about losing his daughter to measles in 1962, urging parents to vaccinate their children so they would not suffer the same loss.
Also, measles is not just a rash illness — about 1 in 5 infected people require hospitalization, and complications like pneumonia or encephalitis can occur. And that’s not even considering the amount of money spent on treatments, hospitalizations, and complications, some lasting a lifetime, such as possible immune system suppression, brain damage from encephalitis, hearing loss, tinnitus, and vision loss.
The measles virus has been studied for generations.
Signs and Symptoms
This is the part turning our “if” into a “when.” Measles doesn’t announce itself. It sneaks in. The symptoms unfold in a way that makes early recognition tricky.
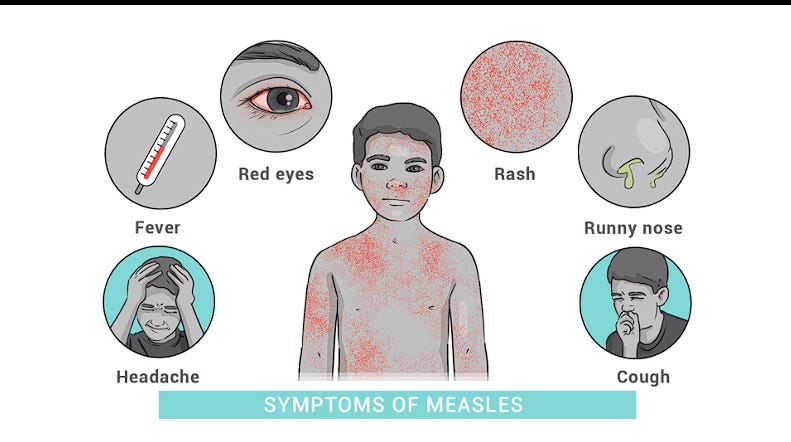
The first few days look a lot like those of other respiratory illnesses. Infected kids may develop a fever, along with the “three Cs” of measles, as doctors call them: cough, coryza (runny nose), and conjunctivitis (red, watery eyes).
As our nurse told us, this is how measles gets into schools. At this stage, parents—or the kids themselves—just “Advil up” and head to school. In our district, like many others, students aren’t allowed to carry medicine—even over-the-counter pain relievers. So, as our nurse put it, these kids crash around lunchtime, when the medicine wears off, and the symptoms come roaring back.
Around this time, another sign may appear: Koplik spots, tiny bluish-white dots along the inside of the cheeks. They show up a day or two before the rash.
The measles rash usually begins near the hairline or behind the ears, then spreads downward across the face, neck, and torso before reaching the arms and legs. The spots often merge together into larger blotchy patches as the illness progresses.
Here’s the problem: people are contagious before the rash appears.
A student whose early symptoms can be Advil’d away?
They’ve likely already been contagious for a day or more.
A student can feel sick for several days—fever, cough, watery eyes—while already spreading the virus to others in the room. By the time the rash makes the diagnosis obvious, the exposure has most likely already happened.
Teachers are not trained to diagnose illnesses. That’s not our job.
But we are often the adults who see the same students for hours in the same room, day after day. Recognizing when something looks unusual—and getting the school nurse involved—can make a real difference in how quickly a situation is contained.
But the odds are stacked against us, partially by design, and partially because the measles virus is such an efficient little bastard, and we’ve got about 30 other plates to keep spinning on any given day.
Below is a quick visual guide to what measles symptoms actually look like.
The Key Point
People with measles are contagious before the rash appears.
By the time the rash makes the diagnosis obvious, exposure may already have happened. If a student has a fever, cough, red eyes, and looks unusually sick, it’s worth looping in the school nurse.
What Measles Means in a School
If measles enters a school, the biggest problem isn’t just the illness. It’s what happens next.
The measles component of the MMR vaccine is extremely effective—about 97% protection after two doses. In a well-vaccinated school community, most students and staff will never become seriously ill. But we can no longer guarantee a well-vaccinated school community, even in public schools, and even in states with legal requirements for vaccinations before enrollment. Exemptions—medical, religious, or otherwise—have consequences. As a result, to quote my own district, planning for “not if, but when” is a reasonable approach.
Once a case appears, public health responses move quickly. If someone in a school is diagnosed with measles, the local health department begins contact tracing. They determine who may have been exposed and whether those individuals have documented immunity. Hence, the HR/legal-sounding email staff in my district received last week.
Anyone who cannot show proof of immunity—either vaccination records or confirmed prior infection—may be excluded from school for up to 21 days after the last exposure. That window comes from the virus’s incubation period, which can last up to three weeks. Public-health officials are essentially waiting to see whether symptoms appear.
Personally—and we already lost two weeks to snow in February—I can’t imagine prepping lessons and remote work for students who miss three weeks of class. Yes, some of it can be done remotely. But despite school districts crowing otherwise, pandemic remote learning was largely a systematic and structural failure. It. Doesn’t. Work.
Students’ anxiety rises, parents start calling, class progress derails, administrators scramble—and teachers will be expected to make it work. Even if very few people actually get sick, the disruption spreads quickly.
But I Thought Vaccines…
And you’re right. Vaccines are incredibly effective. Two doses of MMR provide about 97% protection, and vaccinated students and staff are remarkably well protected. But occasionally, breakthrough cases occur, and vaccinated individuals still become infected. It’s rare, but it can happen.
When that happens, the illness is usually much milder, and the immune system clears the virus faster. That reduces both the severity of the disease and the likelihood of spreading it to others.
If a vaccinated person develops measles, isolation typically lasts four days after the rash appears, when they are most infectious. After that period, and once symptoms are improving, they are usually cleared to return.
Vaccinated and exposed? Documented vaccination usually prevents the 21-day exclusion. Individuals simply monitor for symptoms.
Not vaccinated—or unable to show immunity—and exposed? That’s where the possible 21-day exclusion comes in.
Public health officials have known for nearly a century: the more people vaccinated, the better the protection for the entire community, including those who cannot be vaccinated for health- or immune-system-related reasons. This is the principle of herd immunity. When vaccination rates stay very high (around 95% or more for measles), the virus struggles to gain a foothold and outbreaks burn out quickly.
Which brings us to the quiet system that kept this from happening very often for the last half-century.
Why Is This Even Happening Now?
The virus circulating today is not a new super-variant chewing through immunity. It’s the same virus we’ve known for a long time. Unlike COVID in 2020, measles isn’t novel. We understand how it spreads—and, until recently, we had largely stopped it in its tracks.
For most of the last half-century, measles was something American schools simply didn’t see very often. That wasn’t luck. It was the result of very high vaccination coverage, sustained for decades after the measles vaccine was introduced in 1963 and later incorporated into the MMR vaccine.
For many years, the United States maintained a vaccination rate of around 95%. In 2000, measles was declared eliminated in the United States, meaning the virus was no longer spreading continuously inside the country. Cases still appeared occasionally, usually brought in by international travelers, but they were quickly contained.
For a long time, the system worked.
So why are we talking about measles in schools again?
The short answer is declining vaccination coverage in some communities.
National vaccination rates remain fairly high overall, but in recent years they have slipped slightly. Kindergarten vaccination coverage for MMR has dropped from around 95% before the pandemic to closer to 92–93% today, according to the Centers for Disease Control and Prevention. For measles, epidemiologists estimate that about 95% community immunity is needed to reliably prevent outbreaks.
That might not sound dramatic. But for a virus as contagious as measles, a few percentage points matter. Just as important, the decline hasn’t happened evenly. Immunity has become patchy.
Some communities still have extremely high vaccination rates. Others have clusters of exemptions or lower coverage. When measles finds one of those gaps, it can spread quickly.
Historically, measles outbreaks in the United States tend to occur in under-vaccinated communities, including:
areas with high rates of vaccine exemptions
close-knit communities where vaccine skepticism spreads socially
populations with limited access to routine health care
Measles doesn’t spread randomly. It spreads where immunity has thinned.
International travel also plays a role. Measles continues to circulate widely in many parts of the world, and travelers occasionally bring the virus back to the United States. When vaccination coverage is high, those imported cases usually go nowhere. When coverage dips, they can ignite outbreaks.
None of this means vaccines have stopped working. In fact, the opposite is true. The measles vaccine remains one of the most effective vaccines ever developed. Two doses provide about 97% protection, and communities that maintain high vaccination rates rarely see significant spread.
What has changed is not the virus, but rather the system around it.
Vaccination rates have slipped in some places. Exemptions have grown in others. Routine childhood care was disrupted during the pandemic, and some families never quite caught back up. None of these changes seems dramatic on their own. But when they accumulate, they reopen doors that had been closed for decades.
Which is how we end up having faculty meetings about measles again.
And it’s worth saying this plainly: it doesn’t have to be this way.
The tools that nearly eliminated measles from American schools still exist. The question is whether we continue using them.
So What Do Teachers Do With This?
Most teachers are not epidemiologists. We’re not writing vaccination policy, and we’re not setting exemption rules.
But we are adults who see the same kids, in the same rooms, for hours every day. When something unusual shows up—fever, cough, red eyes, a student suddenly looking far sicker than the usual late-winter crud—we’re often the first to notice.
That doesn’t make us diagnosticians. It just makes us observers.
And right now it’s spring break season.
Which means that over the past couple of weeks, millions of students have been doing what students do during spring break: traveling. Beaches, theme parks, airports, concerts, and hotels—places where people from all over the country and the world mix together.
Some of my own students are returning from trips to places like Florida, Texas, and South Carolina—states where vaccination coverage has dipped in some communities and where recent measles activity or vulnerability to outbreaks has raised concerns. None of that means they’re bringing measles back with them. But it does mean they just spent a week mixing in a dense soup of humanity.
On top of the usual teacher worries—missing assignments, half-finished projects, kids returning with the academic equivalent of jet lag—a quiet public-health worry is now humming in the background.
If measles does show up in a school, the playbook is straightforward: loop in the nurse, follow the health department’s guidance, and keep teaching while the system around us does what it’s supposed to do.
But it’s worth remembering something bigger: for decades, American schools barely had to think about measles at all. A quiet, boring system of immunization records and routine pediatric visits kept the virus from gaining a foothold in schools.
That system didn’t disappear overnight. It’s just grown thinner in places—eroded by skepticism, misinformation, and flat-out denial of the science.
Which means the meeting I sat through before spring break—the one where the district told us measles was not an if but a when—isn’t really about a virus. It’s about whether we want to keep doing the simple things that kept it out of schools for fifty years.
The science hasn’t changed.
The virus hasn’t changed.
The only question now is what happens next.
Because spring break ends, busloads of kids start showing up at schools again, and a whole lot of students who just spent a week in the wider world will walk back into classrooms.
Let’s see where this goes.




I wish I hadn't read this. But also glad I did.
They closed two schools in my district for a couple days last month due to measles. Yikes.